HENRICO COUNTY, Va. -- When we first met Kathy Campbell outside the Canterbury Rehabilitation and Healthcare Center in Henrico in March 2020, we watched her receive some scary news.
Her brother, John Kozak, had just tested positive for COVID-19.
"When we heard that my world just dropped because I really did not think he was gonna make it at that point," Campbell said.
Kozak never experienced any symptoms, but within a matter of weeks, 51 fellow residents died from COVID.
"There's a lot of people in there that I knew that are now gone," Campbell said.
Canterbury was one of the first nursing homes on the East Coast to be ravaged by the virus.
Even though her brother survived, Campbell said the isolation of the past year has been brutal.

"He's not where he was a year ago, and it's scary to watch and scary to know that you're not in there," Campbell said. "I don't think he's interested in anything going on at all with family or anything anymore."
A recent window visit illustrated Campbell's concern.
"Today I asked him if he wanted to speak to his daughter and he said no, and that's not my brother, he was never like that," Campbell said. "When he said no it just broke my heart."
Former medical director shares his story
"You can't ignore the fact that isolation and the lack of personal contact and touch have also done its damage," Dr. Jim Wright, the former medical director at Canterbury, said.
Dr. Wright said that separation and detachment have been just as harmful as the virus itself.
"I think it has been responsible for a lot of declines, worsening dementia symptoms, weight loss, and deaths in facilities," Wright said.
Wright said he left Canterbury last summer after being told he was going to be stripped of most of his responsibilities.
He had been at Canterbury for 10 years.
He said he believed the decision had to do, at least in part, with his candor during the outbreak.
"I really wanted to make sure the public knew our story from the inside," Wright said.
Reflecting on what happened, Wright recalls watching the virus move from China to Europe to the West Coast, and finally the DC-area.
"We knew it was coming down I-95 from DC and Northern Virginia," Wright said.
But he said facilities did not have the test tubes to put COVID swabs into rendering them unable to test for the virus.
On top of that, the Virginia Department of Health required facilities to test for everything else before even considering COVID.
"What I remember from those first three weeks is fluorescent lights, patients in rooms struggling for breath, not enough nurses, not enough CNAs, not enough PPE, everybody doing everybody's jobs," Wright said.
On March 19, Wright got the news he had been dreading: a resident had tested positive for COVID-19.
"For me, it was simply a call to action, just realizing that it was there and I wasn't going to be getting much sleep, days off were gone, I assembled my team," Wright said.
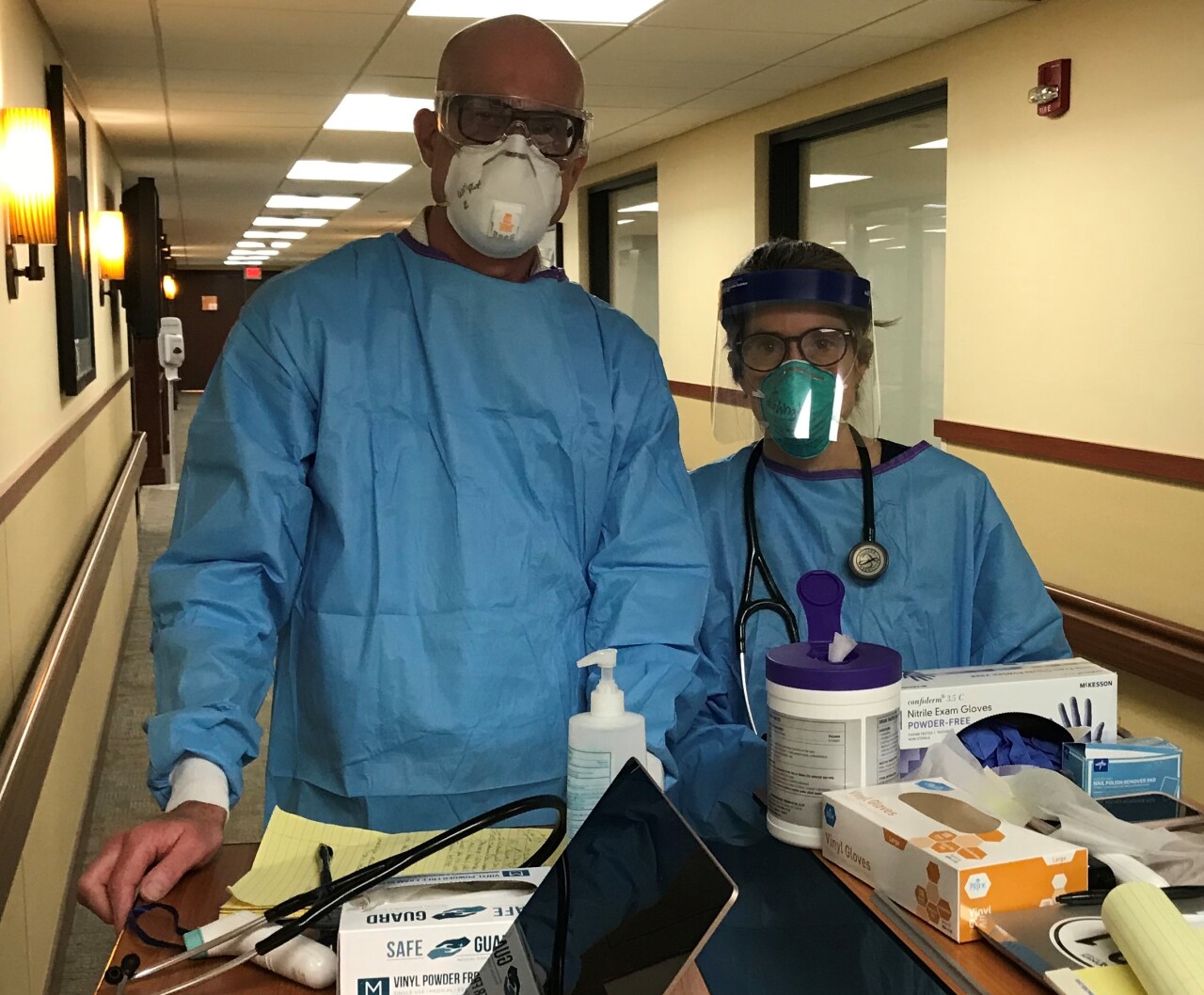
Wright said the fear factor was high among staff.
"It was partially responsible for our poor staffing, nurses and aides simply would not come in, and I do not blame them," Wright said.
He said the anxiety, combined with an already low staffing ratio at Canterbury, ramped up the spread of COVID, which is something numerous studies have born out over the past year.
High staff turnover rates and poor staffing levels likely contributed to high COVID mortality rates in nursing homes, according to the studies.
"I don't think we are different from anyone else, we are a publicly funded, publicly supported nursing home," Wright said about Canterbury. "Our chronic understaffing, which is the same as any other publicly funded nursing home, is driven by the necessity of saving cost."
Wright is now advocating for changes to the industry, while Campbell waits for a day when she can finally go inside of Canterbury to check on her brother and give him a hug.
We requested an interview with someone at Canterbury, but they declined.
The facility's new administrator, Matthew Brooks, told us Dr. Wright was not "let go" or "fired" from Canterbury.
He said they've increased wages across the board, increased transportation options for employees, and increased the availability of testing for staff and residents.
Brooks said all three have led to a significant increase in new hires.
Depend on CBS 6 News and WTVR.com for exclusive Problem Solvers Investigations from our award-winning team of investigative journalists. If you have a story idea, email our team at ProblemSolvers@wtvr.com.or click here to submit a tip.
Find unique, award-winning stories every day on CBS 6 News:











